中国防痨杂志 ›› 2022, Vol. 44 ›› Issue (11): 1205-1212.doi: 10.19982/j.issn.1000-6621.20220276
收稿日期:2022-07-25
出版日期:2022-11-10
发布日期:2022-11-03
通信作者:
李浩
E-mail:lihaocau@cau.edu.cn
基金资助:Received:2022-07-25
Online:2022-11-10
Published:2022-11-03
Contact:
Li Hao
E-mail:lihaocau@cau.edu.cn
Supported by:摘要:
结核病是由结核分枝杆菌复合群引发的人畜共患病,甘露糖帽修饰的脂阿拉伯甘露聚糖(mannose-capped-lipoarabinomannan,ManLAM)是结核分枝杆菌细胞壁上重要的成分,具有免疫调节作用,能够被固有细胞和适应性细胞所识别。作为结核病诊断的生物标记物,存在于体液的ManLAM具有较好的特异性,有区分结核分枝杆菌潜伏感染和活动性结核病的潜力,对于不能获取痰液的结核病患者也具有一定的检测价值。笔者系统介绍ManLAM的结构、生物合成及ManLAM的相关抗体等,并对其在结核病诊断中的研究进展进行总结,以期为结核病诊断技术的研发提供参考。
中图分类号:
唐明慧, 李浩. 脂阿拉伯甘露聚糖的结构功能及其在结核病诊断中的应用[J]. 中国防痨杂志, 2022, 44(11): 1205-1212. doi: 10.19982/j.issn.1000-6621.20220276
Tang Minghui, Li Hao. Structure and function of lipoarabinomannan and its application in tuberculosis diagnosis[J]. Chinese Journal of Antituberculosis, 2022, 44(11): 1205-1212. doi: 10.19982/j.issn.1000-6621.20220276

图2
脂阿拉伯甘露聚糖的结构与生物合成及相关抗体结合表位 注 Manp:吡喃甘露糖苷;D-Araf:D-阿拉伯糖苷;MTX-Man2帽:5-甲硫基-D-木呋喃糖-二甘露糖帽;MPI:甘露糖基磷脂酰肌醇;PI:磷脂酰肌醇;LM:脂甘露聚糖;ManLAM:甘露糖帽修饰的脂阿拉伯甘露聚糖;Ac1PIM2:一酰化磷酸肌醇二甘露糖苷;Ac1PIM4:一酰化磷酸肌醇四甘露糖苷;Man:甘露糖;Ac:酰基化;Ara4:四阿拉伯糖苷;Ara6:六阿拉伯糖苷;甘露糖基转移酶:PimA、PimB’、PimC、PimE、MptA和 MptB;阿拉伯呋喃糖基转移酶:EmbC、AftD、ArafT;甘露糖帽合成酶:CapA和 MptC
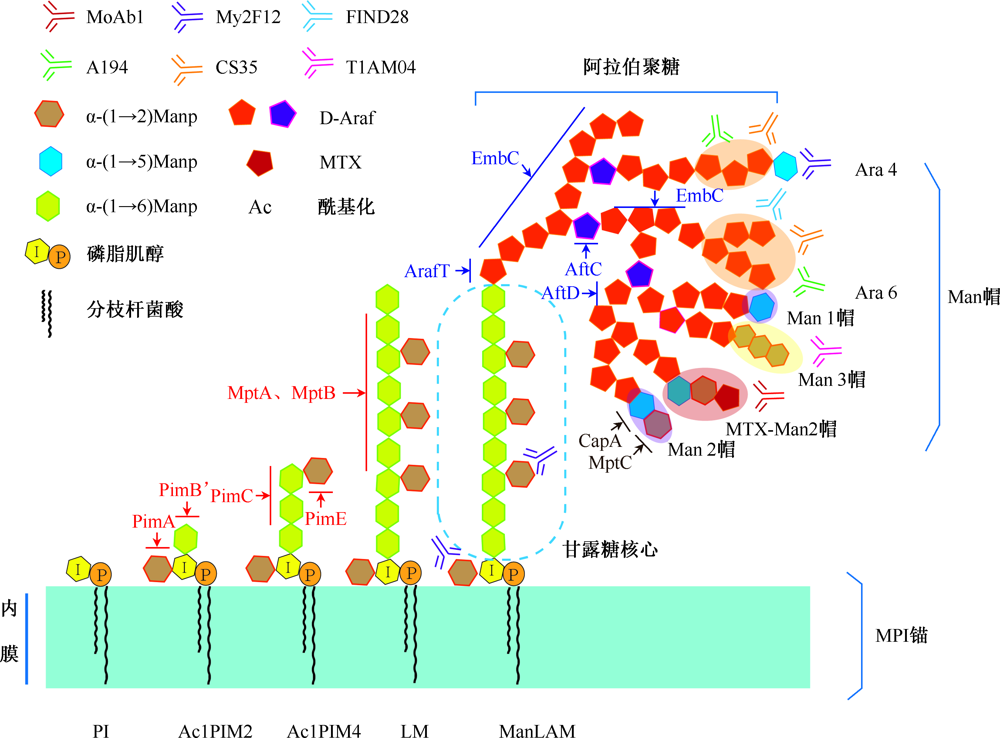
表1
针对ManLAM的单克隆抗体
| 抗体名称 | 抗体来源 | 亚型 | 筛选方式 | 菌株及其抗原 | 识别表位 | 交叉反应 | 检测限 | 参考文献 |
|---|---|---|---|---|---|---|---|---|
| CS-35 | 鼠源性抗体 | IgG3 | 杂交瘤技术 | 麻风分枝杆菌全细胞以及粗提糖脂 | LAM、LM、AM的Ara6(优先)、Ara4、Ara5 | 同时识别ManLAM和LepLAM,但不识别PILAM | 12 pg/ml | [ |
| CS-40 | 鼠源性抗体 | IgG3 | 杂交瘤技术 | 从结核分枝杆菌毒株Erdman纯化的LAM | Manp、MTX衍生物为帽的Ara4和Ara6结构 | 识别ManLAM和PILAM | - | [ |
| 906.7 | 鼠源性抗体 | IgG3 | 杂交瘤技术 | 麻风分枝杆菌 | 不加帽的Ara4和Ara6 | 识别PILAM和LepLAM,对ManLAM识别较弱 | 2ng/ml | [ |
| FIND28 | 鼠源性抗体 | IgG1 | 杂交瘤技术 | 结核分枝杆菌标准株H37Rv | Ara6的Man帽 | 识别ManLAM,能区分非结核分枝杆菌 | 6pg/ml | [ |
| My2F12 | 人鼠嵌合抗体 | IgG1 | 噬菌体展示技术 | - | 含α-(1→2)Manp | 识别ManLAM,不识别PILAM | 2ng/ml | [ |
| MoAb1 | 兔源性抗体 | IgG1 | 噬菌体展示技术 | 卡介苗 | MTX修饰的Man2和Man3帽 | 只识别ManLAM | 12pg/ml | [ |
| S4-20 | 兔源性抗体 | IgG1 | 噬菌体展示技术 | 卡介苗 | 结核分枝杆菌H37Ra的MTX修饰的Man2帽 | 识别ManLAM,能区分非结核分枝杆菌 | 11pg/ml | [ |
| BJRbL01 | 兔源性抗体 | IgG | 噬菌体展示技术 | 结核分枝杆菌标准株H37Rv的细胞壁 | - | 识别ManLAM,能区分非结核分枝杆菌 | 100pg/ml | [ |
| T1AM04 | 人源性抗体 | IgG1 | 单个B细胞筛选技术 | 结核分枝杆菌标准株H37Rv | AM的Ara4和Ara6的Man3 | 识别ManLAM,能区分非结核分枝杆菌 | 10μg/ml | [ |
| T1AM09 | 人源性抗体 | IgG1 | 单个B细胞筛选技术 | 结核分枝杆菌标准株H37Rv | AM的阿拉伯糖苷区域 | 识别ManLAM,能区分非结核分枝杆菌 | - | [ |
| A194 | 人源性抗体 | IgG1 | 单个B细胞筛选技术 | 结核分枝杆菌 | Ara4、Ara6、Manp残基 | 识别ManLAM、LepLAM、PILAM | 13pg/ml | [ |
表2
结核分枝杆菌ManLAM的相关检测
| 检测样本 | 检测方法 | 样本处理 | 信号放大工具 | 捕获和检测抗体 | 检测限 | 参考文献 |
|---|---|---|---|---|---|---|
| 血清 | ELISA与SERS | 高氯酸 | AuNP和ERL | 906.7 | 2ng/ml | [ |
| 尿液 | 夹心ELISA | 蓝藻凝集素、磁珠孵育 | 蓝藻凝集素 | FIND25、FIND28、FIND170 | 1.14ng/ml | [ |
| 尿液 | 夹心ELISA | 蛋白酶K | 水凝胶纳米笼铜络合物染料 | CS35、CHCS9-08 IgG3、A194 | 3ng/ml | [ |
| 尿液与血清 | ECL免疫测试 | 热灭活 | - | FIND28和S4-20 | 10pg/ml | [ |
| 尿液 | FLISA | - | 等离子体光栅 | BPM101和BPM102 | 1fg/ml | [ |
| 尿液 | 生物感受器 | - | AuNP | 抗ManLAM的IgG和IgM | 1~10fg/ml | [ |
| [1] |
Furin J, Cox H, Pai M. Tuberculosis. Lancet, 2019, 393(10181): 1642-1656. doi: 10.1016/s0140-6736(19)30308-3.
doi: S0140-6736(19)30308-3 pmid: 30904262 |
| [2] |
高磊, 张慧, 胡茂桂, 等. 基于多中心调查数据和空间统计模型的全国结核分枝杆菌潜伏感染率估算. 中国防痨杂志, 2022, 44(1): 54-59. doi: 10.19982/j.issn.1000-6621.20210661.
doi: 10.19982/j.issn.1000-6621.20210661 |
| [3] |
Sabur NF, Esmail A, Brar MS, et al. Diagnosing tuberculosis in hospitalized HIV-infected individuals who cannot produce sputum: is urine lipoarabinomannan testing the answer? BMC Infect Dis, 2017, 17(1): 803. doi: 10.1186/s12879-017-2914-7.
doi: 10.1186/s12879-017-2914-7 pmid: 29282005 |
| [4] |
Steingart KR, Ng V, Henry M, et al. Sputum processing methods to improve the sensitivity of smear microscopy for tuberculosis: a systematic review. Lancet Infect Dis, 2006, 6(10): 664-674. doi: 10.1016/S1473-3099(06)70602-8.
doi: 10.1016/S1473-3099(06)70602-8 pmid: 17008175 |
| [5] |
贾红彦, 董静, 张宗德, 等. 结核分枝杆菌感染的免疫学检测技术研究进展及临床应用现状. 中国防痨杂志, 2022, 44(7): 720-726. doi: 10.19982/j.issn.1000-6621.20220103.
doi: 10.19982/j.issn.1000-6621.20220103 |
| [6] |
Park M, Kon OM. Use of Xpert MTB/RIF and Xpert Ultra in extrapulmonary tuberculosis. Expert Rev Anti Infect Ther, 2021, 19(1): 65-77. doi: 10.1080/14787210.2020.1810565.
doi: 10.1080/14787210.2020.1810565 URL |
| [7] |
Correia-Neves M, Fröberg G, Korshun L, et al. Biomarkers for tuberculosis: the case for lipoarabinomannan. ERJ Open Res, 2019, 5(1): 00115-2018. doi: 10.1183/23120541.00115-2018.
doi: 10.1183/23120541.00115-2018 |
| [8] |
Kawasaki M, Echiverri C, Raymond L, et al. Lipoarabinomannan in sputum to detect bacterial load and treatment response in patients with pulmonary tuberculosis: Analytic validation and evaluation in two cohorts. PLoS Med, 2019, 16(4): e1002780. doi: 10.1371/journal.pmed.1002780.
doi: 10.1371/journal.pmed.1002780 |
| [9] |
Mishra AK, Driessen NN, Appelmelk BJ, et al. Lipoarabinomannan and related glycoconjugates: structure, biogenesis and role in Mycobacterium tuberculosis physiology and host-pathogen interaction. FEMS Microbiol Rev, 2011, 35(6): 1126-1157. doi: 10.1111/j.1574-6976.2011.00276.x.
doi: 10.1111/j.1574-6976.2011.00276.x pmid: 21521247 |
| [10] |
Nigou J, Gilleron M, Puzo G. Lipoarabinomannans: from structure to biosynthesis. Biochimie, 2003, 85(1/2): 153-166. doi: 10.1016/s0300-9084(03)00048-8.
doi: 10.1016/s0300-9084(03)00048-8 URL |
| [11] |
Petzold CJ, Stanton LH, Leary JA. Structural characterization of Lipoarabinomannans from Mycobacterium tuberculosis and Mycobacterium smegmatis by ESI mass spectrometry. J Am Soc Mass Spectrom, 2005, 16(7): 1109-1116. doi: 10.1016/j.jasms.2005.02.023.
doi: 10.1016/j.jasms.2005.02.023 URL |
| [12] |
Maeda N, Nigou J, Herrmann JL, et al. The cell surface receptor DC-SIGN discriminates between Mycobacterium species through selective recognition of the mannose caps on lipoarabinomannan. J Biol Chem, 2003, 278(8): 5513-5516. doi: 10.1074/jbc.C200586200.
doi: 10.1074/jbc.C200586200 pmid: 12496255 |
| [13] |
Guerardel Y, Maes E, Elass E, et al. Structural study of lipomannan and lipoarabinomannan from Mycobacterium chelonae. Presence of unusual components with alpha 1,3-mannopyranose side chains. J Biol Chem, 2002, 277(34): 30635-30648. doi: 10.1074/jbc.M204398200.
doi: 10.1074/jbc.M204398200 pmid: 12063260 |
| [14] |
Jankute M, Cox JA, Harrison J, et al. Assembly of the Mycobacterial Cell Wall. Annu Rev Microbiol, 2015, 69: 405-423. doi: 10.1146/annurev-micro-091014-104121.
doi: 10.1146/annurev-micro-091014-104121 pmid: 26488279 |
| [15] |
Pitarque S, Larrouy-Maumus G, Payré B, et al. The immunomodulatory lipoglycans, lipoarabinomannan and lipomannan, are exposed at the mycobacterial cell surface. Tuberculosis (Edinb), 2008, 88(6): 560-565. doi: 10.1016/j.tube.2008.04.002.
doi: 10.1016/j.tube.2008.04.002 URL |
| [16] |
Daffé M, Etienne G. The capsule of Mycobacterium tuberculosis and its implications for pathogenicity. Tuber Lung Dis, 1999, 79(3): 153-169. doi: 10.1054/tuld.1998.0200.
doi: 10.1054/tuld.1998.0200 URL |
| [17] |
Hamasur B, Bruchfeld J, Haile M, et al. Rapid diagnosis of tuberculosis by detection of mycobacterial lipoarabinomannan in urine. J Microbiol Methods, 2001, 45(1): 41-52. doi: 10.1016/s0167-7012(01)00239-1.
doi: 10.1016/s0167-7012(01)00239-1 pmid: 11295196 |
| [18] |
Fukuda T, Matsumura T, Ato M, et al. Critical roles for lipomannan and lipoarabinomannan in cell wall integrity of mycobacteria and pathogenesis of tuberculosis. mBio, 2013, 4(1): e00472-12. doi: 10.1128/mBio.00472-12.
doi: 10.1128/mBio.00472-12 |
| [19] |
Gaylord H, Brennan PJ, Young DB, et al. Most Mycobacterium leprae carbohydrate-reactive monoclonal antibodies are directed to lipoarabinomannan. Infect Immun, 1987, 55(11): 2860-2863. doi: 10.1128/Iai.55.11.2860-2863.1987.
doi: 10.1128/iai.55.11.2860-2863.1987 pmid: 3312018 |
| [20] |
Zhou KL, Li X, Zhang XL, et al. Mycobacterial mannose-capped lipoarabinomannan: a modulator bridging innate and adaptive immunity. Emerg Microbes Infect, 2019, 8(1): 1168-1177. doi: 10.1080/22221751.2019.1649097.
doi: 10.1080/22221751.2019.1649097 URL |
| [21] |
De P, Amin AG, Flores D, et al. Structural implications of lipoarabinomannan glycans from global clinical isolates in diagnosis of Mycobacterium tuberculosis infection. J Biol Chem, 2021, 297(5): 101265. doi: 10.1016/j.jbc.2021.101265.
doi: 10.1016/j.jbc.2021.101265 |
| [22] |
Magni R, Rruga F, Alsaab FM, et al. Lipoarabinomannan antigenic epitope differences in tuberculosis disease subtypes. Sci Rep, 2020, 10(1): 13944. doi: 10.1038/s41598-020-70669-9.
doi: 10.1038/s41598-020-70669-9 pmid: 32811861 |
| [23] |
Treumann A, Feng XD, McDonnell L, et al. 5-methylthiopentose: a new substituent on lipoarabinomannan in Mycobacterium tuberculosis. J Mol Biol, 2002, 316(1): 89-100. doi: 10.1006/jmbi.2001.5317.
doi: 10.1006/jmbi.2001.5317 pmid: 11829505 |
| [24] |
Sigal GB, Pinter A, Lowary TL, et al. A Novel Sensitive Immunoassay Targeting the 5-Methylthio-d-Xylofuranose-Lipoarabinomannan Epitope Meets the WHO's Performance Target for Tuberculosis Diagnosis. J Clin Microbiol, 2018, 56(12): e01338-18. doi: 10.1128/JCM.01338-18.
doi: 10.1128/JCM.01338-18 |
| [25] |
Shi L, Torrelles JB, Chatterjee D. Lipoglycans of Mycobacterium tuberculosis: isolation, purification, and characterization. Methods Mol Biol, 2009, 465: 23-45. doi: 10.1007/978-1-59745-207-6_3.
doi: 10.1007/978-1-59745-207-6_3 |
| [26] |
Corrigan DT, Ishida E, Chatterjee D, et al. Monoclonal antibodies to lipoarabinomannan/arabinomannan-characteristics and implications for tuberculosis research and diagnostics[J/OL]. Trends Microbiol, 2022[2022-07-24]. doi: 10.1016/j.tim.2022.07.001.Online ahead of print.
doi: 10.1016/j.tim.2022.07.001 |
| [27] |
范雨鑫, 刘玫肖, 陈晶晶, 等. 结核分枝杆菌脂阿拉伯甘露聚糖的免疫调节作用和诊断价值. 中国防痨杂志, 2021, 43(8): 847-852. doi: 10.3969/j.issn.1000-6621.2021.08.018.
doi: 10.3969/j.issn.1000-6621.2021.08.018 |
| [28] |
De P, Amin AG, Valli E, et al. Estimation of D-Arabinose by Gas Chromatography/Mass Spectrometry as Surrogate for Mycobacterial Lipoarabinomannan in Human Urine. PLoS One, 2015, 10(12): e0144088. doi: 10.1371/journal.pone.0144088.
doi: 10.1371/journal.pone.0144088 |
| [29] |
Sakamuri RM, Price DN, Lee M, et al. Association of lipoarabinomannan with high density lipoprotein in blood: implications for diagnostics. Tuberculosis (Edinb), 2013, 93(3): 301-307. doi: 10.1016/j.tube.2013.02.015.
doi: 10.1016/j.tube.2013.02.015 URL |
| [30] |
Dheda K, Davids V, Lenders L, et al. Clinical utility of a commercial LAM-ELISA assay for TB diagnosis in HIV-infected patients using urine and sputum samples. PLoS One, 2010, 5(3): e9848. doi: 10.1371/journal.pone.0009848.
doi: 10.1371/journal.pone.0009848 URL |
| [31] |
Brock M, Hanlon D, Zhao M, et al. Detection of mycobacterial lipoarabinomannan in serum for diagnosis of active tuberculosis. Diagn Microbiol Infect Dis, 2020, 96(2): 114937. doi: 10.1016/j.diagmicrobio.2019.114937.
doi: 10.1016/j.diagmicrobio.2019.114937 |
| [32] |
García JI, Kelley HV, Meléndez J, et al. Improved Alere Determine Lipoarabinomannan Antigen Detection Test for the Diagnosis of Human and Bovine Tuberculosis by Manipulating Urine and Milk. Sci Rep, 2019, 9(1): 18012. doi: 10.1038/s41598-019-54537-9.
doi: 10.1038/s41598-019-54537-9 pmid: 31784649 |
| [33] |
Broger T, Tsionksy M, Mathew A, et al. Sensitive electrochemiluminescence (ECL) immunoassays for detecting lipoarabinomannan (LAM) and ESAT-6 in urine and serum from tuberculosis patients. PLoS One, 2019, 14(4): e0215443. doi: 10.1371/journal.pone.0215443.
doi: 10.1371/journal.pone.0215443 |
| [34] |
Nkereuwem E, Togun T, Gomez MP, et al. Comparing accuracy of lipoarabinomannan urine tests for diagnosis of pulmonary tuberculosis in children from four African countries: a cross-sectional study. Lancet Infect Dis, 2021, 21(3): 376-384. doi: 10.1016/S1473-3099(20)30598-3.
doi: 10.1016/S1473-3099(20)30598-3 pmid: 33316214 |
| [35] |
Correia-Neves M, Sundling C, Cooper A, et al. Lipoarabinomannan in Active and Passive Protection Against Tuberculosis. Front Immunol, 2019, 10: 1968. doi: 10.3389/fimmu.2019.01968.
doi: 10.3389/fimmu.2019.01968 pmid: 31572351 |
| [36] |
Yu X, Prados-Rosales R, Jenny-Avital ER, et al. Comparative evaluation of profiles of antibodies to mycobacterial capsular polysaccharides in tuberculosis patients and controls stratified by HIV status. Clin Vaccine Immunol, 2012, 19(2): 198-208. doi: 10.1128/CVI.05550-11.
doi: 10.1128/CVI.05550-11 pmid: 22169090 |
| [37] |
Foote MR, Nonnecke BJ, Beitz DC, et al. Antigen-specific B-cell responses by neonatal calves after early vaccination. J Dairy Sci, 2007, 90(11): 5208-5217. doi: 10.3168/jds.2007-0285.
doi: 10.3168/jds.2007-0285 pmid: 17954761 |
| [38] |
Chen T, Blanc C, Eder AZ, et al. Association of Human Antibodies to Arabinomannan With Enhanced Mycobacterial Opsonophagocytosis and Intracellular Growth Reduction. J Infect Dis, 2016, 214(2): 300-310. doi: 10.1093/infdis/jiw141.
doi: 10.1093/infdis/jiw141 pmid: 27056953 |
| [39] |
Chen T, Blanc C, Liu Y, et al. Capsular glycan recognition provides antibody-mediated immunity against tuberculosis. J Clin Invest, 2020, 130(4): 1808-1822. doi: 10.1172/JCI128459.
doi: 10.1172/JCI128459 pmid: 31935198 |
| [40] |
Watson A, Li H, Ma B, et al. Human antibodies targeting a Mycobacterium transporter protein mediate protection against tuberculosis. Nat Commun, 2021, 12(1): 602. doi: 10.1038/s41467-021-20930-0.
doi: 10.1038/s41467-021-20930-0 pmid: 33504803 |
| [41] |
Perley CC, Frahm M, Click EM, et al. The human antibody response to the surface of Mycobacterium tuberculosis. PLoS One, 2014, 9(2): e98938. doi: 10.1371/journal.pone.0098938.
doi: 10.1371/journal.pone.0098938 |
| [42] |
Chan CE, Götze S, Seah GT, et al. The diagnostic targeting of a carbohydrate virulence factor from M.Tuberculosis. Sci Rep, 2015, 5: 10281. doi: 10.1038/srep10281.
doi: 10.1038/srep10281 URL |
| [43] |
Da Costa CT, Khanolkar-Young S, Elliott AM, et al. Immunoglobulin G subclass responses to mycobacterial lipoarabinomannan in HIV-infected and non-infected patients with tuberculosis. Clin Exp Immunol, 1993, 91(1): 25-29. doi: 10.1111/j.1365-2249.1993.tb03348.x.
doi: 10.1111/j.1365-2249.1993.tb03348.x pmid: 8419082 |
| [44] |
Hunter SW, Gaylord H, Brennan PJ. Structure and antigenicity of the phosphorylated lipopolysaccharide antigens from the leprosy and tubercle bacilli. J Biol Chem, 1986, 261(26): 12345-12351.
pmid: 3091602 |
| [45] |
Kaur D, Lowary TL, Vissa VD, et al. Characterization of the epitope of anti-lipoarabinomannan antibodies as the terminal hexaarabinofuranosyl motif of mycobacterial arabinans. Microbiology (Reading), 2002, 148(Pt 10): 3049-3057. doi: 10.1099/00221287-148-10-3049.
doi: 10.1099/00221287-148-10-3049 URL |
| [46] |
Choudhary A, Patel D, Honnen W, et al. Characterization of the Antigenic Heterogeneity of Lipoarabinomannan, the Major Surface Glycolipid of Mycobacterium tuberculosis, and Complexity of Antibody Specificities toward This Antigen. J Immunol, 2018, 200(9): 3053-3066. doi: 10.4049/jimmunol.1701673.
doi: 10.4049/jimmunol.1701673 pmid: 29610143 |
| [47] |
Chatterjee D, Lowell K, Rivoire B, et al. Lipoarabinomannan of Mycobacterium tuberculosis. Capping with mannosyl residues in some strains. J Biol Chem, 1992, 267(9): 6234-6239.
pmid: 1556132 |
| [48] |
Ishida E, Corrigan DT, Malonis RJ, et al. Monoclonal antibodies from humans with Mycobacterium tuberculosis exposure or latent infection recognize distinct arabinomannan epitopes. Commun Biol, 2021, 4(1): 1181. doi: 10.1038/s42003-021-02714-w.
doi: 10.1038/s42003-021-02714-w pmid: 34642445 |
| [49] |
Yan ZH, Zhao B, Pang Y, et al. Generation of mycobacterial lipoarabinomannan-specific monoclonal antibodies and their ability to identify mycobacterium isolates. J Microbiol Immunol Infect, 2021, 54(3): 437-446. doi: 10.1016/j.jmii.2020.02.005.
doi: 10.1016/j.jmii.2020.02.005 URL |
| [50] |
Lawn SD. Point-of-care detection of lipoarabinomannan (LAM) in urine for diagnosis of HIV-associated tuberculosis: a state of the art review. BMC Infect Dis, 2012, 12: 103. doi: 10.1186/1471-2334-12-103.
doi: 10.1186/1471-2334-12-103 pmid: 22536883 |
| [51] |
Matoga MM, Bisson GP, Gupta A, et al. Urine Lipoarabinomannan Testing in Adults With Advanced Human Immunodeficiency Virus in a Trial of Empiric Tuberculosis Therapy. Clin Infect Dis, 2021, 73(4): e870-e877. doi: 10.1093/cid/ciab179.
doi: 10.1093/cid/ciab179 pmid: 33638976 |
| [52] | World Health Organization. The use of lateral flow urine lipoarabinomannan assay (LF-LAM) for the diagnosis and screening of active tuberculosis in people living with HIV. Geneva: World Health Organization, 2015. |
| [53] |
Bjerrum S, Schiller I, Dendukuri N, et al. Lateral flow urine lipoarabinomannan assay for detecting active tuberculosis in people living with HIV. Cochrane Database Syst Rev, 2019, 10(10): CD011420. doi: 10.1002/14651858.CD011420.pub3.
doi: 10.1002/14651858.CD011420.pub3 |
| [54] |
Broger T, Sossen B, du Toit E, et al. Novel lipoarabinomannan point-of-care tuberculosis test for people with HIV: a diagnostic accuracy study. Lancet Infect Dis, 2019, 19(8): 852-861. doi: 10.1016/S1473-3099(19)30001-5.
doi: S1473-3099(19)30001-5 pmid: 31155318 |
| [55] |
Yin X, Ye QQ, Wu KF, et al. Diagnostic value of Lipoarabinomannan antigen for detecting Mycobacterium tuberculosis in adults and children with or without HIV infection. J Clin Lab Anal, 2022, 36(2): e24238. doi: 10.1002/jcla.24238.
doi: 10.1002/jcla.24238 |
| [56] |
Muyoyeta M, Kerkhoff AD, Chilukutu L, et al. Diagnostic accuracy of a novel point-of-care urine lipoarabinomannan assay for the detection of tuberculosis among adult outpatients in Zambia: a prospective cross-sectional study. Eur Respir J, 2021, 58(5): 2003999. doi: 10.1183/13993003.03999-2020.
doi: 10.1183/13993003.03999-2020 |
| [57] |
Crawford AC, Laurentius LB, Mulvihill TS, et al. Detection of the tuberculosis antigenic marker mannose-capped lipoarabinomannan in pretreated serum by surface-enhanced Raman scattering. Analyst, 2017, 142(1): 186-196. doi: 10.1039/c6an02110g.
doi: 10.1039/c6an02110g URL |
| [58] |
Cox JA, Lukande RL, Kalungi S, et al. Is Urinary Lipoarabinomannan the Result of Renal Tuberculosis? Assessment of the Renal Histology in an Autopsy Cohort of Ugandan HIV-Infected Adults. PLoS One, 2015, 10(4): e0123323. doi: 10.1371/journal.pone.0123323.
doi: 10.1371/journal.pone.0123323 |
| [59] |
Lawn SD, Gupta-Wright A. Detection of lipoarabinomannan (LAM) in urine is indicative of disseminated TB with renal involvement in patients living with HIV and advanced immunodeficiency: evidence and implications. Trans R Soc Trop Med Hyg, 2016, 110(3): 180-185. doi: 10.1093/trstmh/trw008.
doi: 10.1093/trstmh/trw008 URL |
| [60] |
Amin AG, De P, Graham B, et al. Urine lipoarabinomannan in HIV uninfected, smear negative, symptomatic TB patients: effective sample pretreatment for a sensitive immunoassay and mass spectrometry. Sci Rep, 2021, 11(1): 2922. doi: 10.1038/s41598-021-82445-4.
doi: 10.1038/s41598-021-82445-4 pmid: 33536495 |
| [61] |
Panraksa Y, Amin AG, Graham B, et al. Immobilization of Proteinase K for urine pretreatment to improve diagnostic accuracy of active tuberculosis. PLoS One, 2021, 16(9): e0257615. doi: 10.1371/journal.pone.0257615.
doi: 10.1371/journal.pone.0257615 |
| [62] |
Owens NA, Young CC, Laurentius LB, et al. Detection of the tuberculosis biomarker mannose-capped lipoarabinomannan in human serum: Impact of sample pretreatment with perchloric acid. Anal Chim Acta, 2019, 1046: 140-147. doi: 10.1016/j.aca.2018.09.037.
doi: S0003-2670(18)31120-6 pmid: 30482291 |
| [63] |
van der Horst M, Karamchand L, Bauer WS, et al. The cyanobacterial lectin, microvirin-N, enhances the specificity and sensitivity of lipoarabinomannan-based TB diagnostic tests. Analyst, 2021, 146(4): 1207-1215. doi: 10.1039/d0an01725f.
doi: 10.1039/d0an01725f pmid: 33367346 |
| [64] |
Paris L, Magni R, Zaidi F, et al. Urine lipoarabinomannan glycan in HIV-negative patients with pulmonary tuberculosis correlates with disease severity. Sci Transl Med, 2017, 9(420): eaal2807. doi: 10.1126/scitranslmed.aal2807.
doi: 10.1126/scitranslmed.aal2807 |
| [65] |
Wood A, Barizuddin S, Darr CM, et al. Ultrasensitive detection of lipoarabinomannan with plasmonic grating biosensors in clinical samples of HIV negative patients with tuberculosis. PLoS One, 2019, 14(3): e0214161. doi: 10.1371/journal.pone.0214161.
doi: 10.1371/journal.pone.0214161 |
| [66] |
Divagar M, Bandaru R, Janakiraman V, et al. A plasmonic fiberoptic absorbance biosensor for mannose-capped lipoarabinomannan based tuberculosis diagnosis. Biosens Bioelectron, 2020, 167: 112488. doi: 10.1016/j.bios.2020.112488.
doi: 10.1016/j.bios.2020.112488 |
| [67] |
Tang XL, Wu SM, Xie Y, et al. Generation and application of ssDNA aptamers against glycolipid antigen ManLAM of Mycobacterium tuberculosis for TB diagnosis. J Infect, 2016, 72(5): 573-586. doi: 10.1016/j.jinf.2016.01.014.
doi: 10.1016/j.jinf.2016.01.014 URL |
| [68] |
Zhou Y, Xiong H, Chen R, et al. Aptamer Detection of Mycobaterium tuberculosis Mannose-Capped Lipoarabinomannan in Lesion Tissues for Tuberculosis Diagnosis. Front Cell Infect Microbiol, 2021, 11: 634915. doi: 10.3389/fcimb.2021.634915.
doi: 10.3389/fcimb.2021.634915 |
| [1] | 邓国防, 王庆文. 重视风湿性疾病合并结核感染的多学科诊治[J]. 中国防痨杂志, 2022, 44(9): 865-868. |
| [2] | 国家感染性疾病临床医学研究中心/深圳市第三人民医院, 北京大学深圳医院, 中国医学科学院北京协和医院, 中国防痨协会, 《中国防痨杂志》编辑委员会, 深圳市炎症与免疫性疾病重点实验室. 风湿性疾病患者合并结核分枝杆菌潜伏感染诊治的专家共识[J]. 中国防痨杂志, 2022, 44(9): 869-879. |
| [3] | 魏赣辉, 张加成, 邱小伟. 容积CT值量化判断5mm以上肺结核病灶活动性的应用价值[J]. 中国防痨杂志, 2022, 44(9): 934-939. |
| [4] | 吴文琪, 钟剑球, 何娟, 邓国防, 王庆文. 风湿性疾病患者结核分枝杆菌潜伏感染激活机制的研究进展[J]. 中国防痨杂志, 2022, 44(9): 954-959. |
| [5] | 陈秋奇, 韩婷婷, 王庆文, 邓国防. 风湿性疾病合并结核分枝杆菌潜伏感染的诊治进展[J]. 中国防痨杂志, 2022, 44(9): 960-965. |
| [6] | 姚蓉, 陆宇. 抗结核药物贝达喹啉的耐药情况及其耐药机制研究进展[J]. 中国防痨杂志, 2022, 44(9): 973-977. |
| [7] | 谢芳晖, 梁丽, 赵霞, 姚蓉, 雷丽梅, 郭慧, 孟萌, 万彬. 肺结核患者痰标本采集的研究进展[J]. 中国防痨杂志, 2022, 44(9): 978-982. |
| [8] | 卢鹏, 王荣, 刘家松, 刘巧, 丁晓艳, 陆伟, 竺丽梅. 结核菌素皮肤试验诊断结核分枝杆菌潜伏感染学校人群预防性服药临界值的确定[J]. 中国防痨杂志, 2022, 44(8): 797-801. |
| [9] | 丁秀荣, 刘家琛, 陈淑华, 康艳芳, 王晨, 娄金丽. 艾滋病患者合并分枝杆菌血流感染的临床特征分析[J]. 中国防痨杂志, 2022, 44(8): 821-826. |
| [10] | 蒋淑萍, 刘昌伟, 李斌, 徐小琴, 罗文基, 余柏林, 张月. 交叉引物恒温扩增技术在初诊疑似肺结核患者诊断中的应用价值[J]. 中国防痨杂志, 2022, 44(8): 844-848. |
| [11] | 刘晓童, 王安素, 蒋中艳, 娄义姣, 高奉琼, 冯加义, 夏同霞. 结核病患者营养筛查和评估工具研究进展[J]. 中国防痨杂志, 2022, 44(8): 855-859. |
| [12] | 代小伟, 王嫩寒, 陈双双, 杨新宇, 田丽丽, 陈红, 张泓泰, 李传友. 二代测序技术检测临床痰标本中结核分枝杆菌的初步评价[J]. 中国防痨杂志, 2022, 44(7): 669-679. |
| [13] | 中国防痨协会骨关节结核专业分会, 中国华北骨结核联盟, 中国西部骨结核联盟. 布鲁氏菌性脊柱炎诊断及治疗专家共识[J]. 中国防痨杂志, 2022, 44(6): 531-538. |
| [14] | 戴广明, 王芬, 曹廷明, 褚洪迁, 黄海荣, 孙照刚. 实时荧光定量PCR检测不同结核标本及其联合玻璃珠磨菌法检测价值的初步研究[J]. 中国防痨杂志, 2022, 44(5): 450-454. |
| [15] | 吴超玲, 邓国防, 付亮, 袁小亮. 呼出气挥发性有机物在肺部感染性疾病诊断中的研究进展[J]. 中国防痨杂志, 2022, 44(5): 505-511. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||
 京公网安备11010202007215号
ip访问总数: ip当日访问总数: 当前在线人数:
京公网安备11010202007215号
ip访问总数: ip当日访问总数: 当前在线人数:
 本作品遵循Creative Commons Attribution 3.0 License授权许可
本作品遵循Creative Commons Attribution 3.0 License授权许可
